On December 22, the Food and Drug Administration granted emergency use authorization of Paxlovid (nirmatrelvir plus ritonavir), the first antiviral pill for the treatment of COVID-19. Clinical trial participants who received Paxlovid within three days of developing symptoms had an 89% lower risk of hospitalization or death. The authorization comes just time, as the SARS-CoV-2 Omicron variant is spreading rapidly throughout the United States and around the world, but supplies will initially be limited.
Paxlovid, from Pfizer, is authorized for people ages 12 and up who test positive for SARS-CoV-2 (the coronavirus that causes COVID-19), have mild to moderate symptoms that started within the past five days and are at high risk for progression to severe disease. Paxlovid is not intended for people who are at risk for exposure to SARS-CoV-2 (pre-exposure prophylaxis), those who have recently been exposed to someone with the virus (post-exposure prophylaxis) or those who already require hospitalization for severe COVID-19. And it should not be considered a substitute for vaccination.
FDA issued an EUA for Paxlovid for the treatment of mild-to-moderate #COVID19 in adults & pediatric patients (age 12 & older weighing at least 40 kg) w/ positive results of direct SARS-CoV-2 testing, and at high risk for progression to severe #COVID19. https://t.co/HVmpdFDJ7r pic.twitter.com/JjqHaKjORY
— U.S. FDA (@US_FDA) December 22, 2021
“Today’s authorization introduces the first treatment for COVID-19 that is in the form of a pill that is taken orally—a major step forward in the fight against this global pandemic,” Patrizia Cavazzoni, MD, director of the FDA’s Center for Drug Evaluation and Research, said in a news release. "This authorization provides a new tool to combat COVID-19 at a crucial time in the pandemic as new variants emerge and promises to make antiviral treatment more accessible to patients who are at high risk for progression to severe COVID-19."
Despite the availability of highly effective COVID-19 vaccines, there is currently no oral treatment for early disease. Monoclonal antibodies are used to prevent disease progression, but they require injection or IV infusion. Other medications, including remdesivir (Veklury) and dexamethasone, are used to treat hospitalized patients with more severe disease. An oral antiviral from Merck, molnupiravir, was narrowly recommended by an FDA advisory committee in early December, but it has not yet received authorization. The Paxlovid authorization was issued without an advisory committee meeting.
UPDATE: The FDA approved molnupiravir on December 23.
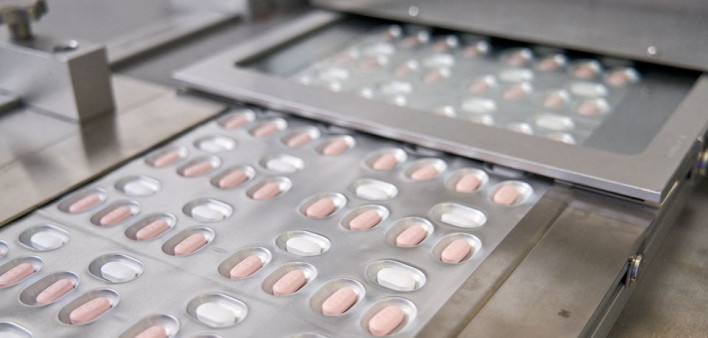
Paxlovid, formerly known as PF-07321332, is a SARS-CoV-2 protease inhibitor that interferes with an enzyme needed for viral replication. Like some HIV protease inhibitors, it is administered with a low dose of ritonavir to maintain higher drug levels in the body. The drug is available by prescription only and requires a positive SARS-CoV-2 rapid antigen or PCR test. It is administered as three tablets (two nirmatrelvir and one ritonavir) twice daily for five days, for a total of 30 pills.
(To put rumors to rest, Paxlovid is not the same as ivermectin, an antiparasitic drug touted—without good evidence—as a treatment for COVID-19. Ivermectin is also a protease inhibitor, but all drugs in this class do not work the same. The HIV protease inhibitor Kaletra (lopinavir/ritonavir), for example, was found to be ineffective against COVID-19.)
“Today’s authorization of Paxlovid represents another tremendous example of how science will help us ultimately defeat this pandemic, which, even two years in, continues to disrupt and devastate lives across the world,” Pfizer CEO Albert Bourla said in a press release. “This breakthrough therapy, which has been shown to significantly reduce hospitalizations and deaths and can be taken at home, will change the way we treat COVID-19, and hopefully help reduce some of the significant pressures facing our healthcare and hospital systems.”
Paxlovid Effectiveness and Safety
The FDA authorization was based on results from the Phase II/III EPIC-HR trial. The study enrolled more than 2,000 non-hospitalized high-risk adults with COVID-19 in North and South America, Europe, Africa and Asia. They tested positive for SARS-CoV-2, had mild to moderate symptoms and were either age 60 or older or had at least one underlying condition associated with progression to severe illness. They had not been vaccinated or had prior SARS-CoV-2 infection. Participants were randomly assigned to receive Paxlovid or a placebo twice daily for five days.
On November 5, Pfizer announced that a planned interim analysis of 1,219 participants showed an 89% reduction in the risk of COVID-19-related hospitalization or death from any cause in people who started treatment within three days of symptom onset. Based on these findings, an independent data and safety monitoring board recommended that the trial be stopped ahead of schedule.
Final data from all 2,246 study participants confirmed the 89% risk reduction when treatment was started within three days and an 88% reduction when it was started within five days. Among patients treated within three days, only five of the 697 who received Paxlovid (0.7%) were hospitalized over 28 days, compared with 44 of the 682 (6.5%) who received the placebo. No Paxlovid recipients and nine placebo recipients died. The relative risk reduction reached 94% for people ages 65 and older, the age group with the highest risk for hospitalization or death. In a second trial of adults who are not at high risk for disease progression, Paxlovid reduced the likelihood of hospitalization by 70%.
Pfizer also announced that SARS-CoV-2 viral load on Day 5 of treatment was approximately 10-fold lower in Paxlovid recipients compared with placebo recipients. What’s more, the company said, recent laboratory data show that Paxlovid remains active against the Omicron variant, which has many mutations in its spike protein that compromise the effectiveness of vaccines and most monoclonal antibodies.
Paxlovid was generally safe and well tolerated. Rates of treatment-emergent adverse events—mostly mild—were comparable in the Paxlovid and placebo arms (23% and 24%, respectively). The most common adverse events are dysgeusia (changes in taste), diarrhea, hypertension and muscle aches. Liver toxicity is a rare serious adverse event, and Paxlovid should be used with caution in people with preexisting liver disease. It should also be used with caution in people with kidney disease. There are currently no data on the use of Paxlovid during pregnancy or lactation. Unlike molnupiravir, a nucleoside analog, Paxlovid did not show evidence of mutagenesis.
The ritonavir used with Paxlovid can interact with many other medications, and doctors and pharmacists should be aware of the risk. Ritonavir is a CYP3A enzyme inhibitor that slows the metabolism and increases levels of some drugs in the body, which can lead to more severe side effects. According to the Paxlovid prescribing information, the new drug should not be used with certain heart disease medications, antibiotics, anticonvulsive drugs, psychiatric medications, statins, sedatives or Viagra (sildenafil). For those taking hormonal contraception, an alternative method is recommended while using Paxlovid. In addition, Paxlovid can increase the toxicity of fentanyl and reduce levels of methadone, leading to opioid withdrawal symptoms.
The prescribing information states that people taking HIV protease inhibitors boosted with ritonavir or cobicistat should continue their treatment and be monitored for increased side effects. The label says the same about ritonavir-containing hepatitis C medications, but the only direct-acting antiviral regimen that includes ritonavir, Viekira Pak (ombitasvir/paritaprevir/ritonavir plus dasabuvir), is no longer used in the United States. The label recommends that Paxlovid not be taken with Mavyret (glecaprevir/pibrentasvir). Paxlovid should not be used—or should be used with caution—in combination with certain cancer medications.
Because ritonavir is active against HIV but is not sufficient to fully control it, people with unsuppressed or undiagnosed HIV who use Paxlovid run the risk of developing resistance to HIV protease inhibitors, which could limit their future treatment options.
Short Supply and Other Challenges
Pfizer said it expects to produce 180,00 courses of Paxlovid this year and more than 120 million in 2022. White House Press Secretary Jen Pasaki said at a news briefing that the government has purchased 10 million courses, at a cost of about $530 each, and will be prepared to distribute them around the country as soon as the supply is available.
White House Press Briefing with @PressSec Jen Psaki - LIVE online here: https://t.co/Wcx6dpoeXa pic.twitter.com/L8hmFKVSy6
— CSPAN (@cspan) December 22, 2021
Tens of thousands of courses are currently ready for delivery, the Washington Post reported, but this won’t be enough to make a dent the growing number of people expected to become infected during the Omicron surge. At least 300,000 additional courses are expected in January and February, when the current surge is expected to be waning. Mike McDermott, Pfizer’s president of global supply, told the Post that it takes about six to eight months to produce a batch of Paxlovid’s active ingredient.
Pfizer said it will offer worldwide access to Paxlovid through a tiered pricing approach based on the income level of each country, under which high-income and upper-middle income countries will pay more than lower-income countries. The company has also signed a voluntary license agreement with the Medicines Patent Pool to help expand access in 95 low- and middle-income countries.
The authorization raises a host of questions about the appropriate use of oral antivirals. Should they be available for everyone with early COVID-19 or only those at high risk for severe disease? How well do they for vaccinated individuals with breakthrough infections? Could they potentially be used for COVID-19 PrEP for immunocompromised people who don’t respond well to the vaccines? And in practical terms, will people be able to get tested for SARS-CoV-2 soon enough to fall within the five-day window after developing symptoms?
But while issues of supply, availability and access remain to be worked out, experts lauded the authorization as a milestone in the COVID-19 crisis.
“Paxlovid will be a true game-changer in every sense of the word,” Monica Gandhi, MD, director of the University of California at San Francisco’s Center for AIDS Research told POZ. “There are adults who remain unvaccinated who are at risk of severe COVID, and this five-day oral medication reduces their risk of hospitalization and death by 88%—almost the same protection afforded by the vaccines. There are those who are immunocompromised and still at risk of a severe breakthrough infection despite vaccination, and this medication will be essential to prevent them from progressing to severe disease, or may even be given as prophylaxis. Today is a huge day in COVID history.”
Click here to read the prescribing information for Paxlovid.
Click here for more news about COVID-19 treatment.






Comments
Comments